The Mamacare360 programme is aimed at goal 3 of the SDGs, good health and wellbeing for all. Working to improve maternal health by promoting Respectful Maternity Care (RMC) for all women during pregnancy, childbirth, and in the time after birth, WBFA sees the link between pregnant women and their primary health givers as vital to their health after delivery and that of their newborn. Respectful maternity care is a universal human right due to every childbearing woman in every health system around the world (WRA, 2010). We believe that: “Midwifery is a vital solution to the challenges of providing high-quality maternal and newborn care for all women and newborn infants in all countries. It is also an effective means to promote the health and wellbeing of women of childbearing age, as well as their newborns and families, with a potentially rapid and sustained effect on population health outcomes.” (Lancet Midwifery Series 2014).
The programme delivers care in line with the World Health Organization (WHO, 2016) recommendations for pregnant women to increase the number of contact with healthcare providers throughout their pregnancy, from four to at least eight. Mamacare360 is bridging an identified gap in achieving best outcomes, by making the mother a premium partner in her own outcome, through education and awareness in birth preparedness. The Mamacare360 birth preparedness programme of antenatal and postnatal education and financial inclusion, using the very same tools such as Emergency Obstetrics and Newborn Care (EmONC), client-held Personal Health Records (PHRs) and Respectful Maternity Care (RMC) empowers the mother by engendering health information and education, during that key eleven-month (antenatal and postnatal) nest and nurture period.
Through this innovative flagship programme launched in 86 WBFA’s MamaCare360 Antenatal and Postnatal Education Programme delivered through our well-trained 55-midwives-strong team, provides mothers and families with critical information on their pregnancy, nutrition, birth preparedness finance and care of the baby. The uniqueness of this programme lies in its delivery through WBFA-trained midwives at health care facilities across several states in the country.
In hard-to-reach facilities, WBFA has ensured that the Midwives come from the communities in which they serve, in order to build trust and bring help to the doorsteps of our primary stakeholders. Our work shows that providing women and their families with information at the grassroots is a critical significant change for improved health outcomes for communities and the nation at large.
Through development and distribution of the now ubiquitous clean delivery Mamakit, which has been adopted, replicated, and amplified so widely across the country, we ensure that every pregnant woman has sanitary and sterile delivery materials with her, to encourage hospital deliveries.
In 2013 the Wellbeing Foundation Africa commissioned a research study in Kwara State that identified ignorance and lack of education; Poor access to transportation to Primary Health care facility; Strong cultural and traditional belief systems including financially incentivised traditional birth attendants (TBAs); strong influence by parents and husband; Avoidance of suturing, episiotomy, and repeated vaginal examination; A belief that anaesthetics hinder wounds from healing fast and naturally; Perception that they are in better control of the delivery process, and what happens to them when they are at home, unlike being restricted to the ethics that guide Doctors in the hospitals; Some feel more comfortable at home where they can be around their family; Celebrations at the birth of the child are more easily done at home; in addition to the cost associated with delivery; as some of the reasons why pregnant women do not utilise medical facilities during and after pregnancies.
With an estimated 560 maternal deaths per 100,000 live births, Nigeria currently is the largest contributor to maternal deaths in sub-Saharan Africa and the second largest contributor, globally.
Maternal mortality occurs from risks attributable to pregnancy and childbirth and obstetric haemorrhage, eclampsia, sepsis, obstructed labour, and complications of unsafe abortions are some of the most common causes of maternal deaths in Nigeria.
Low levels of facility-based delivery, skilled attendance at birth and use of modern contraceptive methods contribute to the newborn mortality ratio which is also very high, 37 newborn deaths for every 1000 live births, and 42 of every 1000 pregnancies resulting in stillbirths. Deaths of newborns represent one third deaths of children under the age of five in Nigeria (WHO, 2013). Over $1.5bn is lost in productivity due to maternal mortality every year in Nigeria.
Globally, the Sustainable Development Goals (SDGs) have set an ambitious target of reducing global maternal mortality ratio to less than 70,000 per 100,000 live births by 2030. In Nigeria, the adoption of the Safe Motherhood Initiative, the integrated maternal, newborn and child health (IMNCH) strategy, and the establishment of Midwife Service Scheme (MSS) are just some of the few strategies put in place to curb the high rate of deaths at birth.
Impact
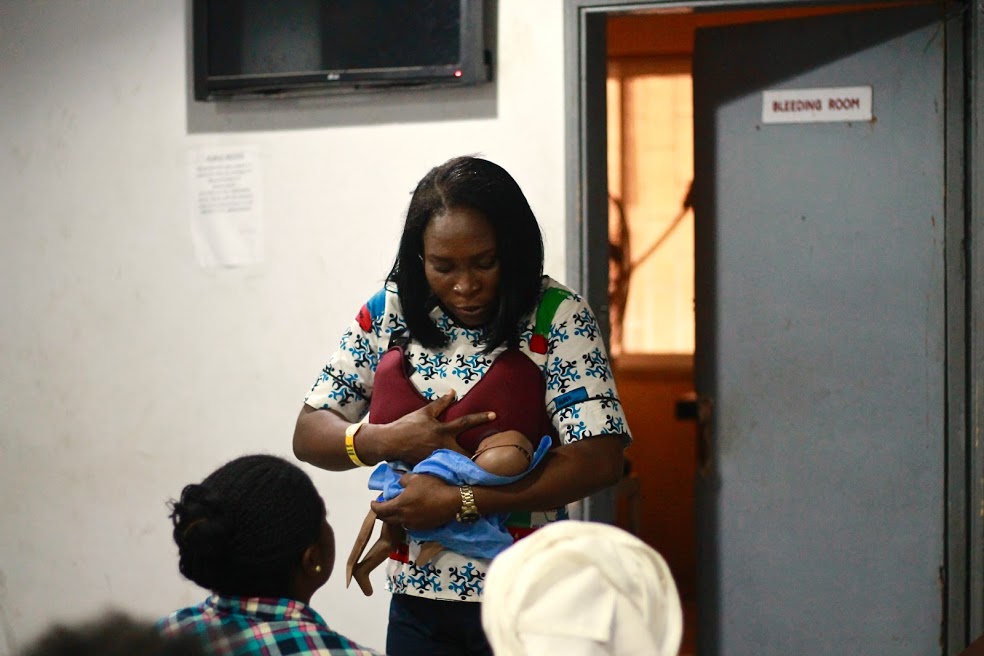
Parent Education Training Programme
Pregnancy, birth and early childhood are crucial times in most parents’ lives. It is the time when the baby develops in response to his/her early experiences and the foundation for future life is laid down. At Wellbeing Foundation, we recognise the importance of this period and provide antenatal and postnatal education programmes sometimes known antenatal classes to help prepare mothers for birth, give them confidence to go through labour, and care for their babies. The programme provides a range of information and topics include; preparation for birth, labour, coping with pain, care of the newborn and breastfeeding. The classes are fun, informative and led by a qualified midwife. Women expecting twins are encouraged to attend classes early, from 24 weeks pregnancy. The classes are a good way to make friends with other parents who are expecting babies around the same time.
Opportunities
As the pandemic continues to ravage the world, its impact on the lives of vulnerable populations is being assessed to include a widening of the preexisting gaps of inequality especially with respect to the delivery of healthcare services. Restrictions imposed by governments have threatened to negatively impact the uptake of health care services especially in rural areas as patients weigh the risks of showing up at healthcare facilities to receive attention. This trend puts the gains made in previous years at risk as women and adolescent girls revert to dangerous cultural practices to seek relief.
In response to this, WBFA has identified the need to expand on the following areas:
- Recruitment of more midwives
- Expand the programme to more healthcare facilities and healthcare service delivery areas.
- Recruitment and training of new health workers
- Home-care service and follow up
- Strengthen advocacy to community influencers especially on Adolescent PSHE & RR
Telemedicine e.g: Mamacare360 WhatsApp groups, WBFA Mamacare360 Chatbot
